Email : admin@mskdoc.co.nz | Phone : 02727 00100
Opening Hours : Mon-Friday : 10 AM – 4 PM
Email : admin@mskdoc.co.nz | Phone : 02727 00100
Opening Hours : Mon-Friday : 10 AM – 4 PM
Email : admin@mskdoc.co.nz | Phone : 02727 00100 | Opening Hours : Mon-Friday : 10 AM – 4 PM
By: Dr Zaid Matti
Musculoskeletal Medicine Specialist
Abdominal pain is a common complaint among patients, often leading to extensive investigations, unnecessary surgical procedures, and significant emotional distress. Among the numerous conditions causing abdominal pain, Abdominal Cutaneous Nerve Entrapment Syndrome (ACNES) stands out as a frequently overlooked yet notably common condition, affecting up to 30% of patients presenting with chronic abdominal pain (Clarke & Kanakarajan, 2015).

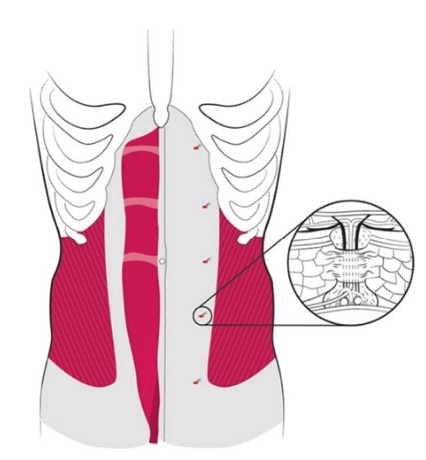
ACNES occurs due to compression or irritation of the small sensory nerves in the abdominal wall. These nerves, particularly the anterior cutaneous branches of the thoracoabdominal nerves (T7–T12) and the iliohypogastric nerve (T12, L1), run through narrow fibrous channels within the rectus abdominis muscles. Entrapment typically occurs at points where nerves change direction, pass through muscular tunnels, or traverse fibrous tissue bands (Clarke & Kanakarajan, 2015).
Patients with ACNES often experience localized pain, which is sharp, burning, or stabbing. The pain may radiate along the nerve’s path, occasionally mimicking other conditions such as thoracic radiculopathy. Notably, pain tends to increase with muscle contractions or movements like coughing, sitting up, or physical exercise. Sensory disturbances such as numbness, tingling, or heightened sensitivity in the affected area are also common (Clarke & Kanakarajan, 2015).
Women are more frequently affected, with a reported female-to-male ratio as high as 5:1. Common triggers include previous abdominal surgeries, pregnancy, sports activities involving the abdominal muscles, and scar tissue formation (Clarke & Kanakarajan, 2015).
Accurate diagnosis involves a thorough clinical history, physical examination, and diagnostic interventions:
Carnett’s Sign: Pain intensifies when abdominal muscles are tensed, helping differentiate abdominal wall pain from internal abdominal conditions.
Hover Sign: Pain elicited by pressing specific nerve passages in the abdomen.
Local Anesthetic Injection: Injection at the suspected site that significantly reduces pain confirms the diagnosis (Clarke & Kanakarajan, 2015).
Early recognition of ACNES is crucial. Delayed diagnosis often leads to the development of central sensitization, increasing overall pain sensitivity and significantly impacting patients’ quality of life. Early intervention can spare patients extensive and unnecessary testing, surgeries, and psychological distress (Clarke & Kanakarajan, 2015).
Management of ACNES ranges from conservative measures to advanced interventions:
Conservative Measures: Education, stretching exercises, avoidance of triggering activities, and pain-relief medications (e.g., topical lidocaine or capsaicin creams).
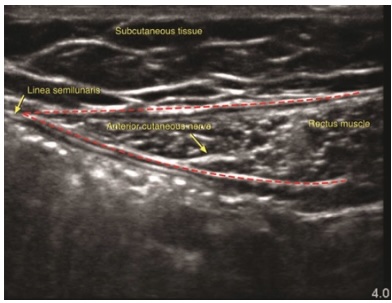
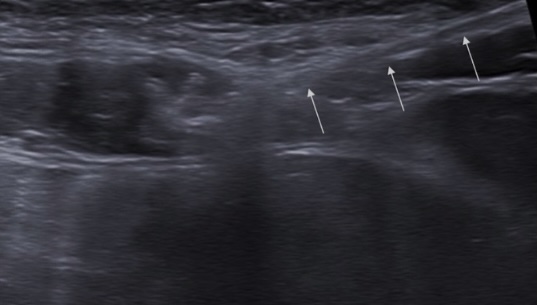
Minimally Invasive Treatments: Ultrasound-guided injections of local anesthetics and corticosteroids, providing targeted relief and reducing inflammation.
Advanced Interventions: Radiofrequency treatments to reduce nerve sensitivity, and in severe cases, surgical neurectomy (nerve removal) for definitive relief (Clarke & Kanakarajan, 2015).
Recent studies support the efficacy of ultrasound-guided injections, which provide precise pain relief lasting several weeks and minimize procedural discomfort (Clarke & Kanakarajan, 2015)
Awareness of ACNES among healthcare providers and patients is paramount for timely diagnosis and effective treatment. Recognizing this syndrome prevents unnecessary procedures, reduces patient anxiety, and significantly improves clinical outcomes. As clinicians, our role includes not only treating the physical symptoms but also addressing the psychological and emotional impact through education and supportive care.
For patients experiencing persistent abdominal pain, exploring the possibility of ACNES with a knowledgeable healthcare provider can be a life-changing step towards recovery and enhanced quality of life.
References: Clarke, S., & Kanakarajan, S. (2015). Abdominal cutaneous nerve entrapment syndrome. Continuing Education in Anaesthesia, Critical Care & Pain, 15(2), 60-63.